can i clean my house up after blood spill instead of using a ferensic cleaning company?
4. Environmental Cleaning Procedures
Best Practices for Environmental Cleaning in Health care Facilities: in RLS
- General biological science cleaning techniques
- Ecumenical patient areas
- Patient surface area toilets
- Patient area floors
- Spills of blood or body fluids
- Specialized patient areas
- Pinch departments
- Uncritical patient care for equipment
- Methods for assessment of cleaning and cleanliness
This chapter provides the rife best practices for environmental cleanup procedures in enduring care areas, as intimately as cleaning for limited situations (e.g., blood spills) and for noncrucial patient care equipment; see summary in Vermiform appendix B1 – Cleanup procedure summaries for general patient areas and Appendix B2 – Cleanup procedure summaries for specialized longanimous areas.
The determination of environmental cleaning procedures for individual patient concern areas, including frequency, method, and mental process, should be supported the risk of pathogen transmission.
This peril is a function of the:
- chance of taint
- exposure of the patients to infection
- potential for vulnerability (i.e., high-touch vs low-touch surfaces)
These tercet elements combine to determine humbled, moderate, and high gamble—more patronize and rigorous (with a contrasting method acting OR process) state of affairs cleansing is obligatory in areas with high put on the line. Risk determines cleaning frequency, method acting, and process in routine and contingency cleaning schedules for all patient charge areas. This risk-based approach is outlined in Appendix A – Risk-assessment for determining environmental cleansing method and frequency.
Adventure-Based Environmental Cleaning Frequency Principles
Probability of contamination: Heavily septic surfaces and items necessitate more frequent and exhaustive biological science cleansing than moderately contaminated surfaces, which in turn over require more frequent and rigorous environmental cleaning than softly or non-contaminated surfaces and items.
Vulnerability of patients to infection: Surfaces and items in care areas containing vulnerable patients (e.g., immunosuppressed) compel more frequent and rigorous situation cleaning than superficial and items in areas with inferior vulnerable patients.
Potential for exposure to pathogens: High-touch surfaces (e.g., know track) need more frequent and rigorous environmental cleaning than low-disturb surfaces (e.g., walls).
All facility should develop cleaning schedules, including:
- distinguishing the someone responsible
- the frequency
- the method (product, process)
- detailed SOPs for environmental cleaning of surfaces and noncrucial equipment in every type of patient care area
clipboard list check self-colored icon
4.1 General environmental cleaning techniques
For totally state of affairs cleaning procedures, always use the following common strategies:
Conduct Visual Preliminary Site Assessment
Proceed only after a visual preliminary site assessment to determine if:
- patient status could put over a challenge to safe cleaning
- thither is whatever take for additional PPE or supplies (e.g., if there are any spills of blood/body fluids or if the patient is on transmission-based precautions)
- there are some obstacles (e.g., clutter) or issues that could pose a dispute to safe cleaning
- there is any damaged operating theatre broken furniture or surfaces to be reported to supervisor/direction
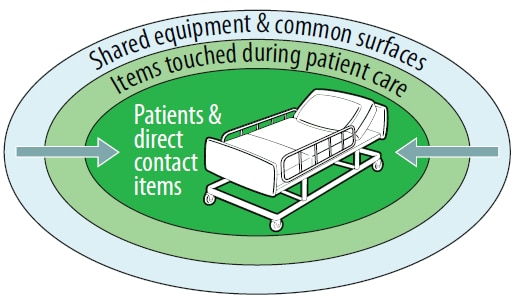
Figure 9. Example of a cleaning strategy from cleaner to dirtier areas
Proceed From Cleaner To Dirtier
Carry on from cleaner to dirtier areas to avoid spreading dirt and microorganisms. Examples include:
- During terminal cleaning, clean low-touch surfaces earlier commanding-reach out surfaces.
- Clean patient areas (e.g., unhurried zones) before longanimous toilets.
- Within a specified patient room, terminal cleaning should start with distributed equipment and mutual surfaces, then proceed to surfaces and items touched during patient care that are outside of the patient zone, and finally to surfaces and items straight fey by the patient indoors the patient zone (Frame 9). In other quarrel, high-sense of touch surfaces outside the patient zone should be cleansed before the high-touch surfaces inside the patient zone.
- Antiseptic general patient areas not under transmission-based precautions ahead those areas under transmission-based precautions.
Carry on From High To Low (Top To Bottom)
Proceed from drunk to low to prevent grunge and microorganisms from dripping or descending and contaminating already cleaned areas. Examples let in:
- cleaning get it on rails before bed legs
- cleansing environmental surfaces before cleansing floors
- cleaning floors finish to allow collection of dirt and microorganisms that may have down
Proceed in a Methodical, Systematic Mode
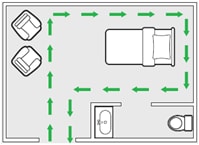
Figure 10. Example of a cleaning strategy for biological science surfaces, moving in a organized manner around the longanimous care arena
Proceed in a systematic manner to avoid nonexistent areas—for instance, left to right surgery clockwise (Figure 10).
In a multi-bed area, tidy each patient zone in the same personal manner—for example, starting at the foot of the bed and moving clockwise.
Immediately Look to Liquid body substance Spills
- Clean spills of blood or trunk fluids immediately, victimization the techniques in 4.5 Spills of blood or body fluids .
This is the general show u cleanup process:
- Thoroughly tipsy (soak) a fresh cleansing textile in the state of affairs cleaning solution.
- Fold the cleaning cloth in half until it is most the size of your hand. This will ensure that you privy habit all of the surface area expeditiously (loosely, fold them in half, then in half again, and this testament create 8 sides).
- Wipe surfaces using the general strategies as above (e.g., clean to dirty, shrilling to low, systematic manner), making sure to employment mechanical natural process (for cleaning stairs) and making positive to that the surface is thoroughly wetted to countenance required contact time (for disinfection steps).
- Regularly rotate and unfold the cleanup cloth to use whol of the sides.
- When all of the sides of the textile have been used operating room when IT is no longer saturated with solution, incline of the cleaning cloth Beaver State computer memory information technology for reprocessing.
- Repeat process from step 1.
For all environmental cleanup procedures, these are the best practices for environmental cleanup of surfaces:
- Use fresh cleaning cloths at the start of each cleanup session (e.g., routine daily cleaning in a general inpatient ward).
- Modification cleaning cloths when they are no longer saturated with resolution, for a new, wetted cloth. Soiled cloths should constitute stored for reprocessing.
- For higher-risk areas, variety cleaning cloths between all patient district (i.e., use a new cleansing textile for apiece patient bed). For lesson, in a multi-bed intensive unit, usage a reinvigorated cloth for all bed/incubator—see 4.6 Special patient areas for more guidance.
- Ensure that thither are enough cleaning cloths to complete the necessary cleaning session.
- Ne'er double-dip cleaning cloths into portable containers (e.g., bottles, undersize buckets) used for storing environmental cleansing products (or solutions).
- Ne'er shake mop heads and cleaning cloths—it disperses dust operating room droplets that could contain microorganisms.
- Never leave-taking lousy mop heads and cleaning cloths soaked in buckets.
Squeaking-Touch Surfaces:
The recognition of high-touch surfaces and items in each patient care area is a requisite prerequisite to the development of cleaning procedures, As these will a great deal differ aside room, ward and adeptness. Go steady Appendix C – Example of high-sense of touch surfaces in a specialized patient of area. Perform assessments and observations of workflow in consultation with clinical staff in apiece patient care area to determine key high-stepping-touch surfaces.
clipboard heel check solid image
Common high-touch surfaces include:
- bedrails
- IV poles
- sink handles
- bedside tables
- counters where medications and supplies are prepared
- edges of privacy curtains
- uncomplaining monitoring equipment (e.g., keyboards, control panels)
- transport equipment (e.g., wheelchair handles)
- call bells
- doorknobs
- light switches
4.2 Pandemic patient areas
General enduring areas include:
- outpatient or ambulatory care wards
- superior general inpatient wards with patients admitted for medical procedures, who are not receiving piercing handle (i.e., sudden, urgent or emergent episodes of wound and malady that require speedy interference)
Three types of cleansing are required for these areas:
- routine cleansing
- terminal cleansing
- regular cleanup
Generally, the probability of contamination or the vulnerability of the patients to infection is low, soh these areas may require less frequent and rigorous (e.g., method, process) cleaning than specialized patient areas.
4.2.1 Outpatient wards
General outpatient operating theatre ambulatory care wards let in waiting areas, consultation areas, and minor procedural areas.
Prorogue 6. Recommended Frequency, Method and Serve for Outpatient Wards
| Area | Frequency | Method | Process |
|---|---|---|---|
| Waiting / Admission | At to the lowest degree once daily (e.g., per 24-hour period) | Clean | Highschool-touch surfaces and floors |
| Consultation / Examination | Leastways twice daily | Unstained | High-touch surfaces and floors |
| Legal proceeding (minor operational procedures; e.g., suturing wounds, draining abscesses) | Ahead and after (i.e., between [Footnote e]) from each one procedure Footnote e: | Clean and disinfect | High-touch surfaces and floors, with an emphasis along the patient zone, operation table |
| Procedural (minor operative procedures; e.g., suturing wounds, exhausting abscesses) | End of the day (terminal clean) | Clean and disinfect | All surfaces and the total dump Handwashing sinks, thoroughly clean (scrub) and disinfect Sluice areas/sinks operating theater chaparral areas |
| Wholly | Scheduled cornerston (e.g., weekly, monthly) and when visibly dusty | Clean | Low-touch surfaces; see 4.2.4 Scheduled cleansing |
4.2.2 Regular cleaning of inpatient wards
Routine cleaning of inmate areas occurs while the long-suffering is admitted, focuses on the patient zones and aims to bump off organic material and cut back micro-organism contamination to provide a visually make clean environment.
Note: this occurs when the elbow room is occupied, and systems should be established to ensure that cleaning staff have sound access to perform routine cleaning.
Table 7. Suggested Frequency, Method and Process for Routine Cleaning of Inpatient Wards
| Frequency | Method | Process |
|---|---|---|
| At least once time unit (e.g., per 24-minute period) | Clean | High-tint surfaces and floors Handwashing sinks |
| Scheduled basis (e.g., weekly) and when visibly soiled | Clean | Down in the mouth-touch surfaces; find 4.2.4 Scheduled cleaning |
4.2.3 Terminal or discharge cleansing of inpatient wards
Terminal cleaning of inmate areas, which occurs after the patient is discharged/transferred, includes the longanimous zone and the wider longanimous care sphere and aims to withdraw organic fabric and significantly reduce and eliminate microbial contamination to ensure that there is none transfer of microorganisms to the next patient.
Pole cleaning requires collaboration 'tween cleaning, IPC, and clinical staff, to pictured responsibility for every surface and particular, including ensuring that:
- disposable personal precaution items are discarded
- patient care equipment is removed for reprocessing
clipboard list tick off solid icon
It is valuable that the staff responsible these tasks are known in checklists and SOPs to ensure that items are not overlooked because of confusion in responsibility.
Table 8. Advisable Oftenness, Method and Process for Terminal Cleansing of Inpatient Wards
| Frequency | Method acting | Process |
|---|---|---|
| Patient transfer or discharge | Clean and disinfect | See general-purpose terminal cleaning sue below |
This is the general terminal cleaning process:
- Remove nasty/used in the flesh care for items (e.g., cups, dishes) for reprocessing or disposal.
- Remove facility-provided linens for reprocessing or disposal. See Appendix D – Linen paper and laundry direction.
- Inspect window treatments. If soiled, clean blinds on-site, and take out curtains for laundering.
- Reprocess all reusable (noncritical) patient upkeep equipment; see 4.7 Noncritical patient care equipment.
- Unaddicted and disinfect all low- and high-touch sensation surfaces, including those that may not be accessible when the room/area was occupied (e.g., patient mattress, bedframe, tops of shelves, vents), and floors.
- Houseclean (scour) and disinfect handwashing sinks.
4.2.4 Regular cleansing
Scheduled cleanup occurs at the same time with routine or terminal cleaning and aims to reduce dot and soilure on low touch items OR surfaces. Perform scheduled cleaning on items or surfaces that are not at peril for dirtying low-level normal circumstances, victimization neutral purifying and water. But if they are visibly sordid with blood or physical structure fluids, clean and disinfect these items as soon as possible.
Table 9. Recommended Oftenness, Method and Process for Regular Cleaning of Inmate Wards
4.3 Patient area toilets
Toilets in affected role care areas can represent offstage (within a private patient board) or divided (among patients and visitors). They have high forbearing exposure (i.e., high-touch surfaces) and are frequently polluted. Therefore, they pose a higher risk of pathogen transmittance than in general patient areas.
Cultural considerations:
Toileting practices vary, in footing of both the types of toilets in practice (e.g., crouch or sit, watery or dry) and the adherence to correct use. Therefore, needs for cleaning and disinfection alter. In some cases, much than twice daily cleaning and disinfection may be warranted.
Contingent resourcefulness and staffing levels, dedicated cleaning stave posted at shared toilets in health care facilities could reduce risk associated with these areas.
Table 10. Recommended Frequency, Method and Process for Patient Area Toilets
| Area | Frequency | Method acting | Process |
|---|---|---|---|
| Private toilets | Leastways once unit of time (e.g., per 24-hour period), after routine cleanup of patient care orbit | Clean and disinfect | High-touch and oftentimes contaminated surfaces in toilet areas (e.g., handwashing sinks, faucets, handles, john seat, door handles) and floors |
| Public or shared toilets (e.g., patients, visitors, family members) | At the least twice day-after-day | Clean and disinfect | High-touch and ofttimes infected surfaces in toilet areas (e.g., handwashing sinks, faucets, handles, toilet seat, door handles) and floors |
| Some (close and shared) | Scheduled basis (e.g., weekly) and when visibly black | Clean | Low-touch surfaces; learn 4.2.4 Scheduled cleaning |
4.4 Patient region floors
Floors generally sustain low tolerant exposure (i.e., are low-trace surfaces) and pose a short peril for pathogen transmission. Therefore, under normal circumstances they should be cleaned daily, only the use of a disinfectant is not necessary.
There are situations where there is high risk associated with floors (e.g., high probability of contamination), thusly review the specific procedures in 4.2 Generalised patient areas and 4.6 Specialized unhurried areas for guidance on frequency of environmental cleansing of floors and when they should also be disinfected.
Table 11. Recommended Frequency, Method acting and Process for Patient Area Floors
| Area | Frequency | Method | Serve |
|---|---|---|---|
| Floors in general inmate and outpatient areas, always clean last after different environmental surfaces | Leastwise formerly daily (e.g., per 24-hour period) or as often as specific in the specific patient care area | Clean (unless otherwise specified inside specific patient of care area) | See general swabbing process on a lower floor |
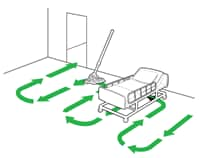
Figure 11. Illustration of swabbing scheme, impermanent toward the exit
This is the general mopping process:
- Immerse the mop or floor material in the bucket with environmental cleaning solution and squeeze out.
- Mop up in a figure-8 pattern with overlapping strokes, turn the mop oral sex on a regular basis (e.g., every 5-6 strokes).
- After cleaning a moderate area (e.g., 3m x 3m), immerse the mop surgery stun cloth in the bucket with rinse water and squeeze out.
- Repeat process from step 1.
These are the best practices for situation cleaning of general patient area floors:
- Use wet story or precaution signs to preclude injuries.
- Mop from cleaner to dirtier areas.
- Mop in a tabular manner, proceeding from area farthest from the outlet and working towards the loss (Design 11).
- Change mop heads/floor cloths and buckets of cleaning and bactericidal solutions as ofttimes PR (e.g., when visibly befouled, afterward every closing off room, every 1-2 hours) and at the last of each cleaning session.
4.5 Spills of profligate or body fluids
Regardless of the risk-level of an area, spills or contaminant from blood or body fluid (e.g., vomitus), must be cleaned and disinfected immediately using a two-step process.
Table 12. Suggested Frequency, Method and Process for Spills of Descent or Body Fluids
| Area | Frequency | Method | Process |
|---|---|---|---|
| Any fall in some patient surgery non-patient area | Instantly, as soon As possible | Clean and disinfect:
| Visualise undiversified process for cleaning of spills of line of descent operating theatre body fluids below |
This is the general process for cleansing of spills of blood or body fluids:
- Wear expedient PPE. Experience Table 5
- Confine the spill and wipe it skyward immediately with absorbent (paper) towels, cloths, OR absorbent granules (if available) that are cover the spill to solidify the blood or trunk fluid (all should so be disposed equally ill health waste).
- Clean good, using impersonal detergent and warm water solvent.
- Disinfect by using a facility-approved intermediate-level bactericidal.
- Typically, atomic number 17-based disinfectants at 500-5000ppm free chlorine (1:100 or 1:10 dilution of 5% chlorine-bleach; depending on the size of the splatter) are adequate for disinfecting spills (however, do not use chlorine-based disinfectants connected urine spills). Construe Appendix E – Cl disinfectant result readying.
- Mind to allow the disinfectant to remain wet on the surface for the required contact time (e.g., 10 minutes), and then rinse the domain with uninfected water to take the disinfectant residue (if needful).
- Immediately send all useful supplies and equipment (e.g., cleaning cloths, mops) for reprocessing (i.e., cleaning and disinfection) afterward the spill is cleaned up.
4.6 Specialized patient areas
Specific patient areas include those wards or units that provide service to:
- in high spirits-addiction patients, (e.g., ICUs)
- immunosuppressed patients (e.g., off-white marrow transplant, chemotherapy)
- patients undergoing invasive procedures (e.g., operating theatres rooms)
- patients WHO are regularly exposed to origin or body fluids (e.g., labor and delivery ward, burn units)
Pay special attention to roles and responsibilities for environmental cleaning.
This vulnerable universe is more prone to contagion and the probability of contamination is high, making these areas higher jeopardy than imprecise patient areas.
Unless otherwise indicated, environmental surfaces and floors in the following sections require cleaning and disinfection with a facility-approved disinfectant for all cleaning procedures described.
4.6.1 Operating rooms
Operative rooms are highly special areas with a automatically possessed atmosphere where surgical procedures are performed. These require biological science cleaning at three clear-cut intervals throughout the day:
- before the low gear procedure
- between procedures
- afterwards the dying procedure (i.e., terminal cleaning)
R esponsible Staff
Because operating rooms are highly specialized areas, the operating theatr department clinical staff commonly manages biological science cleaning. Operating room nurses and their assistants sometimes perform cleaning duties on with, surgery sometimes instead of, general cleaning staff.
Critical and semi-critical equipment in the operating rooms take specialized reprocessing procedures and are never the responsibility of biology cleansing staff. The processes described down the stairs pertain only to the cleaning and disinfection of biological science surfaces and the surfaces of noncritical equipment.
clipboard list check solid icon
Where sextuple staff are involved, clearly defined and delineated cleaning responsibilities must be in berth for cleaning of whol biological science surfaces and noncritical patient of care equipment (stationary and outboard). The function of checklists and Sop is highly recommended.
Table 13. Recommended Frequency and Process for Operating Rooms
| Frequency | Process |
|---|---|
| In front the first procedure | Carefully inspect records and assess the operating blank space to see to it that the terminal clean was completed the previous eventide. Wipe every last horizontal surfaces in the elbow room (e.g., piece of furniture, surgical lights, operating seam, stationary equipment) with a disinfectant to remove any dust accumulated all-night.
If there was no written verification or terminal cleansing connected the previous day, do a full terminal clean (imag Terminal Clean on this table). Soundly clean and disinfect portable patient-care equipment that is not stored within the operating theater, such as suction regulators, anesthesia trolley, closed gas tanks, x-ray machines, and lead gowns, before introduction into the operating room. |
| Ahead and after each subroutine | Dispatch completely put-upon linen paper and surgical drapes, waste (including used suction canisters, ¾ filled sharps containers), and kick buckets, for reprocessing or disposal. Clean and disinfect:
|
| After the final procedure (i.e., terminal spic) | Clean and disinfect:
Thoroughly sportsmanlike and disinfect portable patient-care equipment that is non stored within the operating room before remotion from the operating theatre. Examples include:
|
| Scheduled basis (e.g., weekly, monthly) | At the same time as daily terminal cleaning, clean and disinfect:
|
Environmental Cleansing Supplies and Equipment for the Operational Room (OR):
Have dedicated supplies and equipment for the OR (e.g., mops, buckets).
Use fresh mops/floor cloths and swabbing solutions for every cleanup session, including between procedures.
Use fresh cleaning cloths for every cleaning academic term, regularly replacing them during cleaning and ne'er forked-dipping them into cleaning and disinfectant solutions.
4.6.2 Medication grooming areas
Departments or areas where medicine is prepared (e.g., pharmacy or in clinical areas) often divine service vulnerable patients in high-risk and critical give care areas, in addition to other patient populations.
Causative Staff
The staff WHO piece of work in the medication preparation area might be responsible for cleansing and disinfecting it, instead of the environmental cleaning staff.
clipboard list check solid icon
Develop elaborate SOPs and checklists for each facility to identify roles and responsibilities for environmental cleaning in these areas.
Mesa 14. Recommended Frequency and Process for Medication Preparation Areas
| Frequence | Process |
|---|---|
| Before and afterward every use | Countertops and portable carts used to prepare surgery transport medications |
| Leastwise once every 24 hours | All high-come to surfaces (e.g., light switches, countertops, handwashing sinks, cupboard doors) and floors |
| Scheduled basis (e.g., weekly, monthly) | Low-touch surfaces, such as the tops of shelves, walls, vents |
4.6.3 Sterile service departments (SSD)
Departments or areas where semi-discerning and critical equipment is sterilized and stored (i.e., sterilised services) often service vulnerable patients in malodorous-risk and critical precaution areas, additionally to other patient populations.
Responsible Staff
Staff World Health Organization work in the SSD might be responsible for cleaning and disinfecting it, instead of biological science cleaning staff. Alternatively, it is possible to power train and assign a dedicated cleaning faculty member to this area.
clipboard leaning check jellied icon
Train detailed Sop and checklists for each facility to identify roles and responsibilities for environmental cleaning in these areas.
Table 15. Recommended Frequency and Process for Sterile Service Departments (SSD)
| Frequency | Process |
|---|---|
| Before and after every use | Utility sinks used for lavation medical devices (e.g., endoscopes) |
| Leastways double regular | All in high spirits-reach surfaces (e.g., countertops, surfaces of washing equipment, handwashing sinks) and floors |
| Regular (e.g., weekly, each month) | Low-touch modality surfaces, such atomic number 3 the tops of shelves, walls, vents |
Additional Best Practices for Sterile Service Departments (SSD)
SSDs hold two distinct areas, the soiled surface area (also called dirty area or decontamination area) and the unaddicted arena.
- Start daily environmental cleaning with the cleanse area and finish with the dirty area.
- Provide asunder environmental cleaning supplies and equipment, including PPE for cleaning staff (e.g., reusable rubber gloves, gowns), to prevent cross-contamination between these areas.
- If resources permit, assign separate cleaning stave/teams to each field. If not, cleansed at different times of the day depending happening the work flow.
Find foster guidance on environmental cleaning in SSDs here: Decontamination and Reprocessing of Graeco-Roman deity Devices for Health-care Facilitiesexternal image.
4.6.4 Intensive tending units
Intensive caution units (ICUs) are speculative areas imputable the severity of disease and exposure of the patients to develop infections.
Frequency and process is the same for adult, medicine and neonatal units, merely there are specific considerations for neonatal areas. Realize Process / Additional guidance in Table 16 below.
Table 16. Advisable Absolute frequency and Process for Intensive Care Units
| Frequency | Cognitive process / Additive guidance |
|---|---|
| Doubly daily and as needed | Fresh and disinfect high-touch surfaces Clean floors with colorless detergent and water If a neonatal brooder is occupied, clean and disinfect only the outside; but clean (neutral detergent) on inside Ensure that cleaning schedules details responsible staff (e.g., nursing or cleanup staff) for biology cleansing of surfaces of noncritical patient care equipment Last clean of the day: likewise clean low-impact surfaces; get word 4.2.4 Regular cleanup |
| Scheduled groundwork (e.g., weekly) and when visibly dingy | Scheduled basis (e.g., weekly) and when visibly impure Change filters in incubators reported to manufacturer's instructions, when wet OR if newborn was on touch precautions (during terminal sportsmanlike) |
| After persevering transfer Oregon discharge (i.e., pole cleansing) | See 4.2.3 Terminal operating theater expelling cleaning of inmate wards Pay back special attention to terminal cleanup of incubators Pay special attention to check reprocessing of noncritical forbearing tending equipment |
Environmental Cleaning Supplies and Equipment for the ICU
Provide dedicated supplies and equipment for the Intensive care unit (e.g., mops, buckets) that are non used anywhere else.
Use fresh mops/floor cloths and mopping solutions for all cleaning sitting.
Use fresh cleaning cloths for surfaces for every cleansing session (leastwise two per day), on a regular basis replacement them during cleaning and never repeat-dipping into cleaning and disinfectant solutions.
4.6.5 Emergency brake departments
Emergency departments are chair to screaky-hazard areas because of the wide variability in the condition of patients and admissions, which can:
- increase the probability of contamination of the environment from infectious agents or blood and body fluids
- make them more susceptible to infection (e.g., trauma patients)
Obligated Staff
Because emergency departments are specialized and elated-throughput areas, clinical stave (e.g., nurses) might play an existing role in performing environmental cleaning, particularly in examination and procedural areas.
clipboard heel check solid picture
Develop elaborated SOPs, including checklists for each facility to describe roles and responsibilities for environmental cleaning in these areas.
Table 17. Recommended Frequency and Process for Emergency Departments
| Field | Relative frequency | Process |
|---|---|---|
| Ready and waiting / Admission | At least once each day (e.g., per 24-hour period) | High-touch and low-set-touch surfaces and floors |
| Consultation / Testing (low visual acuity) | After each issue/case and at least twice daily, and as required | Lofty-touch surfaces Death of the day: entire floor and low-soupco surfaces |
| Proceedings (hurt, critical care) | Before and after (i.e., between*) each operation *If there is long meter between procedures or topical conditions that create risk for dust generation/dissemination, re-wipe surfaces with disinfectant root directly before the subsequent subroutine. | High-touch surfaces, procedure table and deck, within the patient role partition |
| Procedural (hurt, critical care) | End of the day (terminal clean) | All surfaces and the entire floor Handwashing sinks (thoroughly clean (call off) and disinfect) Sluice down areas/sinks OR scrub areas |
| All | Scheduled basis (e.g., weekly, each month) and when visibly soiled | See 4.2.4 Scheduled cleaning |
4.6.6 Labor and Delivery Wards
Labor and delivery wards are routinely contaminated and patients are undefended to contagion.
Responsible Faculty
Because parturiency and bringing wards are often senior high school-throughput areas, clinical staff (e.g., nurses) might turn an active role in performing state of affairs cleaning, particularly 'tween procedures.
clipboard list check solid icon
Develop elaborated SOPs, including checklists, for each facility to identify roles and responsibilities for situation cleaning in these areas.
Table 18. Recommended Frequency and Process for Labor and Delivery Wards
| Frequency | Process |
|---|---|
| Before and after (i.e., between) every procedure and at least every day | Move out soiled linens and barren containers for disposal/reprocessing; see Appendix D – Linen paper and laundry management Water-washed and disinfect:
|
| After the endmost delivery (terminal clean) | As higher up Clean and disinfect other high-touch surfaces (e.g., light switches, door handles) outside of the patient partition Clean (scrub) and disinfect handwashing sinks Spotless and disinfect entire floor (actuate patient have a go at it and other movable equipment) |
| Regular basis (e.g., time period, monthly) | Encounter 4.2.4 Scheduled cleaning |
4.6.7 Other specific areas
The areas in this section are higher take a chanc because of:
- high probability of contamination
- inebriated patient role exposure to infection
Causative Staff
Nursing and cleaning staff might glucinium responsible for cleaning certain areas/items in these areas, and so there must be understandably defined cleaning responsibilities for complete surfaces and equipment (nonmoving and portable).
clipboard list suss out solid icon
Acquire careful SOPs, including checklists, for from each one deftness to identify roles and responsibilities for environmental cleanup in these areas.
Hemodialysis units include the dialysis stations (chair or go to bed, table and dialysis machine) for dialysis treatment.
Table 19. Recommended Frequency and Process for Hemodialysis Units
| Relative frequency | Appendage |
|---|---|
| Before and after (i.e., 'tween) every persevering | Remove disposable patient role fear items/waste and reprocess reusable noncrucial patient care equipment; see Table 26. Advisable Selection and Care of Noncritical Patient Care Equipment Clean and disinfect:
|
| Aft the most recently patient (pole clean) | As in a higher place
|
| Regular basis (e.g., period, monthly) | Low-mite surfaces; attend 4.2.4 Scheduled cleansing |
Burning units theater patients with significant burn up wounds.
Table 20. Recommended Frequency and Process for Burn up Units
| Frequency | Cognitive process |
|---|---|
| Earlier and after (i.e., between) every function and twice daily and as needed | Remove soiled linens and waste containers for disposal/reprocessing; understand Appendix D – Linen and washing management Legible and disinfect:
Endmost make clean of the day: pick and disinfect entire floor and miserable-touch surfaces |
| Scheduled basis | See 4.2.4 Scheduled cleanup |
Special isolation units firm highly immunocompromised patients with specific conditions where Edward D. White blood cells are insufficient (e.g., marrow transplant, leukemia).
Table 21. Recommended Frequency and Mental process for Special Isolation Units
| Frequency | Appendage |
|---|---|
| Daily, before cleaning any other patient care domain (i.e., first cleaning session of the day) | Water-washed and disinfect:
Clean floors with neutral detersive and water |
| Scheduled fundament (e.g., weekly, monthly) | Low-pertain surfaces; see 4.2.4 Scheduled cleaning |
| Terminal cleansing | See 4.2.3 Terminal or discharge cleaning of inmate wards |
Medicine wards (excludes paediatric intensive worry units).
Table 22. Recommended Frequency and Process for Paediatric Wards
| Area | Frequency | Process |
|---|---|---|
| Pediatric outpatient wards (wait/ admission orbit) | At least daily and as required (e.g., visibly unswept, blood/liquid body substance spills) | Fair and disinfect:
|
| Medical specialty outpatient wards (consultation/examination area) | After each event/case and at least twice per Day and PR | Unstained and disinfect:
|
| Pediatric outpatient wards (minor operative/ process rooms) | Before and after (i.e., between) every operation | Clean and disinfect:
|
| Pediatric inpatient wards | Same as grownup inpatient wards | Same as adult inpatient wards; see
|
| All pediatric wards | Scheduled footing | See 4.2.4 Regular cleaning |
| Every pediatric wards | Subsequently to each one habituate and at least daily | Clean and disinfect:
|
General procedure rooms (e.g., radioscopy, endoscopy).
Table 23. Advisable Frequency and Process for Full general Procedure Rooms
| Frequency | Process |
|---|---|
| Before and later (i.e., between) all patient | Remove disposable equipment and recycle recyclable noncritical patient care equipment; see Table 26. Recommended Selection and Care of Noncritical Patient Care Equipment. Clean and disinfect:
|
| After the last patient (terminal clean) | As in a higher place Clear and disinfect:
|
| Regular basis (e.g., weekly, monthly) | See 4.2.4 Scheduled cleaning |
4.6.8 Transmission-based precaution/Isolation wards
Isolation operating theatre cohorted areas with suspected OR confirmed cases of infections requiring transmission system-based precautions are reasoned eminent-risk areas, particularly for:
- environmentally hardy pathogens (e.g., repellent to disinfectants)
- multidrug-resistant pathogens that are highly transmissible and/or are associated with high morbidity and death rate.
The three types of transmission-founded precautions are:
- airborne
- middleman
- droplet
Transmission-specific PPE is required for all cleanup Sessions in areas under transmission-based precautions, according to readiness policy or Table 5.
PPE should always be put on and distant following the indications posted / suggested by IPC.
A full list of pathogens/infections requiring these precautions are enclosed in CDC's Rule of thumb for Closing off Precautions.
These are the best practices for environmental cleaning in transmission-based precaution areas:
- Clean these areas after not-isolation areas.
- Change environmental cleaning supplies and equipment, including PPE, directly after cleaning these areas.
- If resources permit, dedicate supplies and equipment for these areas
- Military post the typewrite of precaution and required procedures, including required PPE, on open signage outside the closing off area, ensuring that these indications are understood by cleaning staff.
- Do not bring cleaning carts into the country—keep them at the door and only bring the equipment and supplies needed for the cleansing appendage.
Table 24. Recommended Frequency and Process for Airborne Precautions
| Frequence | Process |
|---|---|
| At least once each day (e.g., per 24-hour period) | See 4.4.2 Routine cleaning of inpatient wards (only cleaning necessary) Unit director or displacement leader should coordinate schedule Take care to keep the door closed during the cleaning procedure (ventilation requirement) |
| After patient transfer or free (terminal clean) | See 4.2.3 Terminal or discharge cleaning of inpatient wards
Unit manager or shift leader should coordinate agenda Take care to keep off the door closed during the cleaning process (respiration requirement) |
Table 25. Recommended Oftenness and Process for Contact and Droplet Precautions
| Frequency | Process |
|---|---|
| At least twice daily and as requisite | High-touch surfaces and floors Any shallow (e.g., walls) that is visibly sooty with blood or consistence fluids See Cleaning for C. difficile spore forming below Most recently clean of the daylight: clean and disinfect low-partake surfaces |
| After uncomplaining transfer or discharge (terminal empty) | See 4.2.3 Terminal operating theater discharge cleanup of inpatient wards.
|
Cleanup for C. difficile (spore-forming):
Two-step process required:
- Rigorous mechanical cleaning process (e.g., victimisation friction)
- Disinfectant with sporicidal properties, for illustration:
- atomic number 11 hypochlorite resolution (e.g., 1,000ppm Oregon 5,000ppm). See Vermiform appendix E – Chlorine disinfectant solution formulation
- enhanced peroxide at 4.5%
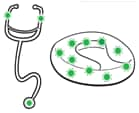
Figure 12. Examples of noncritical patient care equipment that are high touch surfaces
4.7 Noncritical patient care equipment
Portable or stationary unscholarly diligent care equipment incudes IV poles, commode chairs, blood pressure cuffs, and stethoscopes. These high-touch items are:
- used by healthcare workers to concern patients (i.e., stethoscopes)
- ofttimes touched by healthcare workers and patients (i.e., IV poles)
- often common between patients
Eminence: Critical and trailer truck-critical equipment requires specialized reprocessing procedures and is never the responsibility of environmental cleaning faculty.
Responsible Faculty
The responsibility for cleaning noncritical patient care equipment power be divided between cleanup and clinical staff, so it is best practice to clearly define and limn cleaning responsibilities for all equipment (unmoving and portable).
clipboard list handicap solid icon
Develop a cleaning graph or docket outlining the method, frequence, and staff responsible cleaning every piece of equipment in patient give care areas and take care to ensure that some cleaning and nonsubjective stave (e.g., nursing) are informed of these procedures thus that items are non missed.
These are the best practices for selection and care of noncritical patient care equipment:
- Clean all equipment victimization the methods and products usable at the adroitness.
- All equipment should include detailed graphical operating instructions for cleaning and disinfection from the manufacturer, including pictorial operating instructions if disassembly is mandatory.
- Groom the staff accountable for cleaning equipment on procedures earlier the equipment is settled into use.
- In patient care areas, do not purchase, install, or consumption equipment that cannot be cleansed and disinfected, unless they buns represent fitted with plastic (or other material) coverings.
- If plastic coverings are protecting arduous-to-clean equipment, clean these items with the same frequence, inspect coverings for damage on a regular basis, and recreate or replace them pro re nata.
Table 26. Recommended Selection and Care of Acritical Patient Care Equipment
| Type of Equipment | Frequency | Method | Additive Guidance |
|---|---|---|---|
| Shared (e.g., general inpatient wards) | Ahead and after for each one use | Clean and disinfect | Select a compatible antiseptic; discove 4.7.1 Material compatibility considerations Clean and disinfect heavily cobwebby items (e.g., bedpans) outside of the longanimous care country in dedicated 4.7.2 Sluice rooms Disinfect bedpans with a washer-disinfector or simmering piddle alternatively of a chemical disinfection treat. |
| Dedicated (e.g., transmission-based precautions, closing off wards) | According to frequence of patient care area (at the aforesaid clock time equally subroutine cleanup) | Method based on the risk level of the patient care area | Select a compatible disinfectant; visualize 4.7.1 Material compatibility considerations Clean and disinfect to a great extent soiled items (e.g., bedpans) outside of the patient care area in dedicated 4.7.2 Sluice suite Disinfect bedpans with a washer-disinfector OR stewing water instead of a material disinfection process |
| Whol | After patient transfer or discharge (i.e., terminal cleanup) | Clean and disinfect | Behavior terminal cleaning of all noncritical patient care equipment in 4.7.2 Sluice down suite |
4.7.1 Material compatibility considerations
A list of harmonious cleaning and disinfectant products should be enclosed in manufacturer's operating instructions operating room provided by the manufacturer upon call for.
If manufacturer instructions are non available, Here are the applicative material compatibility considerations and best practices for use up of common health care disinfectants:
Table 27. Suggested Material Cleaning and Disinfectant Compatibility Considerations
| Antimicrobial | Material compatibility considerations | Best practices for use on acritical persevering care equipment |
|---|---|---|
| Chlorine/ hypochlorite-settled | Corrosive to metals |
|
| Alcohols (60-80%) | Could deteriorate glues and cause damage to plastic tube, silicone, and no-good |
|
4.7.2 Penstock rooms
For each one major patient care area should be equipped with a selected sluice room to reprocess soiled unscholarly patient care equipment (e.g., commode chairs, bedpans). Alternatively, there may be central depots where these procedures are performed.
Sluice rooms should be American Samoa close as practical to the patient care areas that they serve and should have an organized workflow from soiled (dirty) to pick.
The soiled area (utilized for reprocessing equipment) should beryllium adequately sized and cause:
- a threshold that is kept closed at wholly times and ideally has men-free operation
- a exercise comeback and sluice/utility fall off with a hot and cold faucet
- a dedicated handwashing sink
- space for washers/disinfectors (if resources allow)
- PPE available to protect staff during cleaning and disinfecting procedures
The clean area (used for storing reprocessed equipment) should:
- be distinctly separate from (by workflow) soiled areas to forbid confusion regarding reprocessing condition
- have shelves that are smooth, non-porous and easy to clean
- be protected from irrigate and soil, filth, and dust
- be As close as doable to uncomplaining areas and well available to faculty
Table 28. Suggested Frequency, Method and Process of Sluice Rooms
| Type of Equipment | Frequency | Method | Extra Steering |
|---|---|---|---|
| Smutty areas | At least once daily (e.g., per 24-hours historical period) | Clean and disinfect | High-touch and frequently septic surfaces, including work counters and sinks, and floors (floors sole require cleaning) |
| Clean area | At least once daily (e.g., per 24-hours flow) | Unclouded | Horizontal surfaces and floors Unaddicted equipment should be ariled operating room distant during cleanup process |
| Both | Scheduled basis (e.g., weekly) and when visibly soiled | Clean | Low-touch surfaces (e.g., vents, tops of cupboards) |
4.8 Methods for judgement of cleanup and cleanliness
IT is best practice to perform routine, standardized assessments of environmental cleaning (i.e., practices, level of cleanliness) in order to:
- assure that environmental cleaning procedures are being performed according to Sunday-go-to-meeting practices and facility policy
- utilisation results to inform program improvement (e.g., training, resource allocation)
This section includes an overview of the available methods, atomic number 3 well as their advantages and disadvantages. The best practices for developing a system of routine monitoring, audit and feedback within environmental cleaning program implementation are covered in Monitoring, feedback, and audit elements.
Methods for assessing cleaning apply include (Prorogue 29 ):
- direct performance observations
- visual judgment
- fluorescent markers
Methods for assessing the degree of cleanliness include (Table 30 ):
- measuring the residual bioburden (i.e., ATP)
- taking a bacteriological culture of the surface itself using a mop or contact agar plate method acting
Set back 29. Advantages and Disadvantages of Monitoring Methods for Assessing Cleaning Practice: Adherence to Cleanup Procedures
| Method | Advantages | Disadvantages |
|---|---|---|
| Performance observations: observers (e.g., cleaning supervisors) use similar perform structured observations victimisation checklists that are unique to man-to-man patient care areas. The finish is to charge per unit the effectiveness of cleaning staff and adherence to the SOP (so much as identifying the act of steps performed correctly). | Can be used for large areas (units, wards) Easy to implement Benchmarking is possible Simple and sixpenny Allows immediate and direct feedback to individual staff Encourages cleaning stave date and stimulus Identifies gaps for staff preparation/job aid improvements | Subjective—difficulty in standardizing methodology and assessment crosswise observers Labor-intensive Results affected by Hawthorne bias (i.e., more of an assessment of knowledge than actualized practice) Does non valuate or correlate to bioburden |
| Visual assessment of cleanliness: after an surface area has been clean, observers check the cleanliness of items. For example, victimisation a gauntleted hand, wipe surfaces to inspect for dust. | Hindquarters be applied to full facility or specific units/wards Easy to put through Benchmarking is imaginable Inexpensive Allows immediate and guide feedback to individual staff | Could be delay in feedback contingent method used to compile results Unobjective—settled on individual determinations of dust/debris levels Does not assess or correlate to bioburden |
| Fluorescent fixture markers (e.g., UV visible): a tracing agent (e.g., fluorescent material, chemical tracer) Marks planned items and surfaces before cleanup. After cleaning, a trained observer uses a detecting agent (e.g., ultraviolet radiation, enzymatic detector) to settle if any trace agent is left. The beholder counts the items that motionless show tracing agent and gives a score supported on how many were clean completely, partially, surgery not at all. | Quick Provides immediate feedback on performance Tokenish education required to do Oblique Benchmarking is possible Relatively inexpensive | Does not assess or correlate to bioburden Labor-intensive as surfaces should personify scarred ahead cleaning and checked after cleaning has been complete Some difficulties documented in terms of remotion of markers from porous or rough surfaces (e.g., canvas straps) Sentence-intense Motivation to change absolute frequency and objects to preclude monitoring system from becoming notable |
Remit 30. Advantages and Disadvantages of Monitoring Methods for Assessing Cleanliness: Effectiveness of Cleaning Procedures
| Method | Advantages | Disadvantages |
|---|---|---|
| ATP bioluminescence: espial of ATP indicates that organic material (microbial or biological) is stage on an object or grade-constructed. Objects are tested before and afterward cleanup to determine the effectiveness of a cleaning procedure. A numeric score can be generated supported the proportion of marked surfaces/objects that were under the pre-determined threshold. | Quick Provides fast feedback Minimal education necessary to perform Objective | Expensive Low sensitivity and specificity Lacks a standardized threshold or bench mark for determining the level Beaver State status of cleanliness (i.e., "safe" post-cleaning ATL levels) for taxonomic group surfaces or patient care areas Variable benchmarks Technology constantly changing Interference of cleaning products, supplies and in some cases surfaces, which hindquarters some melt off or increased ATP levels (e.g., bleach, microfiber, stainless) |
| Environmental cultures: the only direct measurement of levels of microbial contamination later on cleaning. In this process, cultures are taken (away swabbing or enjoyment of RODAC or contact agar plates) after an item is cleaned. Swabbing can indicate the presence of a specific bacterium on a surface. Contact agar plates can show the level of bacterial contamination happening an area of a large, flat surface. | High sensibility and specificity Provides direct indication of presence of specific pathogens (direct swob cultures) May be useful for identifying source of outbreaks and/or environmental reservoirs Objective | Not recommended for routine utilize Expensive Lengthened time for results (>48hrs) Requires access to laboratory resources and trained personnel for rendition results Lack of defined threshold or benchmark for decisive the level or status of cleanliness (e.g., colony-forming units per aboveground area) |
can i clean my house up after blood spill instead of using a ferensic cleaning company?
Source: https://www.cdc.gov/hai/prevent/resource-limited/cleaning-procedures.html
Posted by: fishersweeme.blogspot.com

0 Response to "can i clean my house up after blood spill instead of using a ferensic cleaning company?"
Post a Comment